Melbourne Airport is planning a third runway.
So I'm doing a science literature dive into reading the air pollution health impacts of aviation emissions...
You know, that coating you find over your car or house if you live under a flight path...this is soot, black carbon (BC), particulate pollution emissions from aircraft landing and taking off. But it's the particles you don't see that are problematic: Ultra Fine Particles (UFP) sometimes referred to as particulate matter with a size designation often classified as PM2.5, but often even smaller which can reach the furthest alveoli of your lungs..
These pollution particulates are not good for your health. UFPs have a high surface area and a capacity to adsorb a substantial amount of toxic organic compounds.
Studies indicate that the "exposure to aircraft emissions induce pulmonary and systemic inflammation, which potentially contributes to cancer, asthma, respiratory and coronary heart disease." (Bendtsen 2021)
In fact it is calculated that aviation emissions on a global basis cause about 16,000 people to die prematurely every year, and of this number about 5,000 people who live within 20 km of airports are estimated to die prematurely each year.
As Steve H L Yim et al (2015) study says: " primary PM2.5 emissions from aviation are a significant contributor to health risk when airport vicinity exposure is captured."
The study also highlights that the health cost of aviation emissions is actually at a magnitude larger than global aviation fatal accident costs, and on par with aviation's climate costs.
I wonder if Melbourne Airport have done their sums on the extra costs to health of people in the 20km radius of the airport with the extra aviation emissions a third runway will induce?
The No Third Tulla Runway campaign has articulated reasons to oppose development of the third runway. These include:
- Too much noise
- Contribution to global warming
- Loss of Woodland (a threatened ecosystem)
- Dodgy Economics
- Lack of Transparency
These are all relevant reasons to oppose the airport. The missing piece in this analysis is the aviation pollution impacts on air quality and human health at all scales: local, regional and global.
This article seeks to draw attention to some of the science on aviation exhaust emissions, air quality and human health.
Aviation emissions and air quality
A recent study by Irene C Dedoussi (2021) raises Implications of future atmospheric composition in decision-making for sustainable aviation. The author highlights that "Aviation emissions lead to degraded air quality and adverse human health impacts, making air quality one of the leading environmental externalities associated with aviation."
She argues that "the changing atmospheric composition, driven by meteorological and background (non-aviation) emissions changes, results in a changing atmospheric response to emissions."
She describes the main pollutants thus:
The main pollutants associated with aviation's regional and global air quality and human health impacts are fine particulate matter (PM2.5) and ozone. PM2.5 has been considered the main driver being responsible for more than 85% of aviation's air quality impacts, but more recent ozone human health impacts functions indicate that the aviation-attributable human health impacts of ozone may be higher, and can even exceed those of PM2.5 (Eastham and Barrett 2016, Quadros et al 2020). The formation pathways of both pollutants from jet engine combustion by-products are primarily non-linear. While PM2.5 can be directly emitted (e.g. in the form of soot), the majority of aviation-attributable PM2.5 takes the form of secondary PM2.5, consisting of nitrate, sulfate and ammonium. Secondary organic aerosols are estimated to comprise ∼2% of aviation-attributable PM2.5 (Quadros et al 2020), although their formation and human health impacts are still an active area of research, in terms of the scientific understanding, and capabilities to measure and model them. Ozone forms from gaseous emissions of NOx and volatile organic compounds.
Health Costs of Aviation Exhaust pollution at local, regional, global scales
The study by Yim et al (2015) investigated the health impacts and costs of aviation exhaust emissions. It calculated the mortality at a local, regional and global level. The conclusion of the Yim et al (2015) study:
"4. ConclusionsWe produce the first multi-scale global assessment of the air quality and human health impacts of aviation, accounting for both fine particulate matter and ozone, estimating that aviation emissions result in ∼16 000 early deaths each year. We find that PM2.5 exposure causes 87% of early deaths. While cruise emissions dominate causing 75% of early deaths due to aviation emissions, approximately half of early deaths are caused by LTO emissions in North America and Europe—regions with relatively high aviation and airport fuel burn. In contrast, 91% of early deaths are caused by non-LTO emissions in Asia. This suggests that LTO emissions reductions in North America and Europe will provide regional benefits, while the benefits of non-LTO emissions reductions will be diffuse and also felt in Asia.A global total of ∼5000 people who live within 20 km of airports are estimated to die prematurely each year due to aviation emissions, with 38% of airport vicinity early deaths in Europe. Our results suggest, in contrast with previous analyses, that primary PM2.5 emissions from aviation are a significant contributor to health risk when airport vicinity exposure is captured. A significant uncertainty in our estimates of the subgrid contribution to PM2.5 exposure is the aviation BC emissions inventory.Finally we show that the monetized health costs of aviation emissions exceed aviation's fatal accident costs and noise costs by an order of magnitude, and is on the same order as aviation's climate costs for discount rates of 2% and 3% (as are appropriate to climate change costing Johnson and Hope 2012). This suggests that environmental benefits of fuel burn reductions are as much in air quality as they are in climate. Furthermore, this implies that when assessing the environmental impacts of aviation biofuels that result in reductions in emissions, the air quality impacts may be in the same order as the climate impacts. For example, paraffinic biofuels would be expected to eliminate SOx emissions and reduce BC emissions by ∼80% (Speth et al 2015).
The study by Yim et al (2015) only looked at the health impact of aviation exhaust emissions. Roy M Harrison et al (2015), appreciated the positive work in "estimating the magnitude of public health impact at various scales, ranging from local, near airport, regional and global."
Harrison et al (2015) articulated that research needs to be wider to encompass "other sources and processes related to aviation that still need to be accounted for. This includes impacts of nitrate aerosol formed from NOx emissions, but probably more important, are the other airport-related emissions from ground service equipment and road traffic."
Harrison et al identify three areas where aviation pollution and health research is needed:
- comprehensive estimation of PM emissions, including both volatile and non-volatile phases and their partitioning and dilution effects at ambient temperatures.
- Aircraft non-exhaust and other airport-related emissions. Such as from tyre, brake and runway wear. Also auxiliary and ground power units in use to power stationary aircraft, and ground service equipment. The large volumes of road traffic in the form of shuttle buses, taxis, private cars, service vehicles etc, which together generate a large pollutant load
- An extended parameterization and assessment of health impacts. Including incorporating "Disability Adjusted Life Years (Lim et al 2012) or Years of Life Lost (Anenberg et al 2010), which are generally more appropriate metrics as they take into account the number of years lost due to ill-health. Additionally, the substantial burden of morbidity associated with air pollutant exposure should be included in further studies. Finally, although monetary valuation provides a common basis for comparison, there are ethical challenges around the valuation of nonmarket goods, such as ecosystem services."
Review of Health Effects associated with exposure to jet engine emissions
The extensive review of literature by Bendtsen et al (2021) on aviation emissions and health impact especially concerning airport staff and residents living near an airport or under a flightpath (or downwind of a flightpath) is well worth reading.
They report that "Proximity to running jet engines or to the airport as such for residential areas is associated with increased exposure and with increased risk of disease, increased hospital admissions and self-reported lung symptoms."
They conclude that "there is evidence that jet engine emissions have physicochemical properties similar to diesel exhaust particles, and that exposure to jet engine emissions is associated with similar adverse health effects as exposure to diesel exhaust particles and other traffic emissions."
In Summarising Health effect Studies Bendtsen et al (2021) highlighted the health risks for residents in the vicinity of an airport or under flight paths or downwind of flightpaths:
We identified a limited number of studies and one report reporting correlations between airport emission levels and health effects of residents in the vicinity of airports: Aircraft emission levels were associated with increased hospitalization for asthma, respiratory, and heart conditions especially in susceptible subgroups such as children below 5 years of age, elderly above 65 years of age [66, 94] and lower socioeconomic groups [97, 112]. A Dutch report on Schiphol similarly reported that school children and adults took more medication and had more respiratory complaint on days with increased exposure to aircraft emissions and concludes that health effects of air traffic emissions are similar to those caused by road traffic [59]. A biomonitoring study showed increased blood levels of the inflammatory marker IL-6 in volunteers with mild to moderate asthma after a walk in a zone with high levels of aircraft emissions [107]. It is well-known that other types of air pollution including diesel exhaust cause morbidity and mortality [113]. Taken together, these results suggest that the exposure to aircraft emissions induce pulmonary and systemic inflammation, which potentially contributes to cancer, asthma, respiratory and coronary heart disease.
Annual costs of noise, air quality and climate damages
The environmental damages of an airport with noise, air quality and climate change will vary in terms of the size of the airport, the airport operations capacity, and population distance from the airport. Philip J Wolfe et al (2014) goes into some detail on the annual costs of noise, air quality and climate damages.
"Mean expected noise and air quality damages decay with distance from the airport, but for noise, the range of expected damages at a given distance can be high and depends on orientation with respect to runways and flight patterns. Damages from aviation-induced climate change dominate those from local air quality degradation and noise pollution further away from the airport. However, air quality damages may exceed those from climate when considering the impact of cruise emissions on air quality." say the authors.
From the study conclusion:
Noise damages are found to dominate the per person expected environmental impact at near-airport distances (<6 km). Because expected air quality damages are more sensitive to the number of local operations, air quality damages are expected to comprise a greater percentage of the burden at larger airports, eventually overtaking noise as the dominant environmental impact at airports with greater than 1.25 million operations per year. At distances greater than 6 km, damages from climate change or air quality damages from cruise emissions dominate environmental costs. On a per person basis, noise damages dominate as the average person within 5 km of an airport bears $41 a year in damages ($25–59). While noise is currently the primary environmental impact of concern with respect to airport expansion, these results indicate that as airports become larger the impact of concern may shift to air quality. Regional and local scale analyses of aviation environmental impacts are therefore important and should be used to supplement aggregate cost-benefit analyses of aviation environmental policies.
Health impact of Aviation Ultra Fine Particles
Before we go into detail, it is useful to understand Ultra Fine Particles. Kwon et al (2020) in an article published in Nature help us out with this defination:
Ultrafine particles (UFPs) are aerosols with an aerodynamic diameter of 0.1 µm (100 nm) or less. There is a growing concern in the public health community about the contribution of UFPs to human health. Despite their modest mass and size, they dominate in terms of the number of particles in the ambient air. A particular concern about UFPs is their ability to reach the most distal lung regions (alveoli) and circumvent primary airway defenses. Moreover, UFPs have a high surface area and a capacity to adsorb a substantial amount of toxic organic compounds. Harmful systemic health effects of PM10 or PM2.5 are often attributable to the UFP fraction.
As part of a study by Neelakshi Hudda et al (2020), Impacts of Aviation Emissions on Near-Airport Residential Air Quality, outlines some of the health impacts of aviation emissions.
Recently, the impacts of aviation emissions on ground-level ambient ultrafine particle (UFP; aerodynamic diameter < 100 nm) concentrations were found to extend over unexpectedly large areas near airports and in particular along flight paths. 24
For example, elevated particle number concentrations (PNC) were reported downwind of major international airports as far as 7 km near Amsterdam, 7.3 km in Boston, 18 km in Los Angeles, and 22 km in London. 25−29 UFPs are emitted at high rates by jet aircraft 30 and linked to increased rates of hypertension and cardiovascular morbidities. 31,32
However, UFPs do not contribute significantly to mass in the fine particle range and are not routinely monitored, in part due to a lack of ambient air quality standards. Therefore, they present the possibility of being an additional important confounder for near-airport epidemiological investigations. 33,34
For example, Wing et al. 35 found that UFP exposure was. independently associated with adverse birth outcomes in the vicinity of Los Angeles International Airport.
Similarly, black carbon (BC) and oxides of nitrogen, which are also emitted at high rates by aircraft 30,36−38 and have recognized adverse cardiovascular effects, 39 are also elevated near airports. 24,25
Some near-airport epidemiological studies have accounted for confounding pollutants, like fine (PM 2.516 ) and coarse particulate matter (PM 1015,40,41 ), ozone, 16 and NO 2 , 41 but by using regional-scale central monitor data or predictive models that only account for larger-scale spatial patterns and ground-transportation emissions. Confounding co-exposure to aviation-origin emissions themselves remains unaccounted for, limiting the causal interpretation of the epidemiological results.
A study by Lammers et al (2020) conducted within 500 metres of Schiphol Airport (Amsterdam) and near two major roads set out to determine short term impact of Ultra Fine Particles (UFP) emanating from aviation emissions and larger Particulate Matter from two nearby major roads. Ultra fine particles appeared to reduce lung function, while larger particulates from major road pollution increased blood pressure. The study drew the conclusion:
Short-term exposure to high levels of UFP near Schiphol Airport was, on average, associated with decreased lung function (mainly FVC) and prolonged repolarization of the heart (QTc), directly after exposure in young healthy adults. The effects were relatively small, however, they appeared after single exposures of 5 h in a young healthy population. As this study cannot make any inferences about long-term health impacts, studies investigating potential health effects of long-term exposure to airport-related UFP, are urgently needed.
Neelakshi Hudda et al (2014) in a study - Emissions from an International Airport Increase Particle Number Concentrations 4-fold at 10 km Downwind - examined the spatial pattern of particle number (PN) concentrations downwind from the Los Angeles International Airport (LAX).
We measured at least a 2-fold increase in PN concentrations over unimpacted baseline PN concentrations during most hours of the day in an area of about 60 km2 that extended to 16 km (10 miles) downwind and a 4- to 5-fold increase to 8–10 km (5–6 miles) downwind.
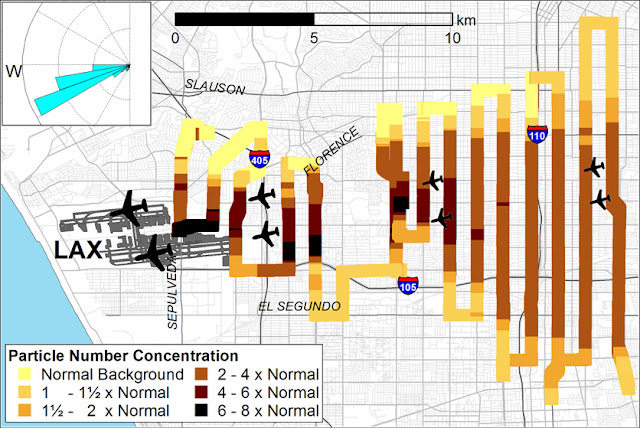 |
| Source: Hudda et al (2014), Emissions from an International Airport Increase Particle Number Concentrations 4-fold at 10 km Downwind |
It is clear particular pollution impact for Melbourne airport with a third runway will be much more than the noise impact from flight paths.
Melbourne Airport reported Pollution and projected pollution with and without a 3rd Runway for NOx, PM10, PM2.5, and VOCs
Chapter B10 deals with Air Quality in the Major Development Plan for the 3rd Runway. It lists current pollution levels, plus projected pollution levels for No Build scenario and a #rd runway build scenario.
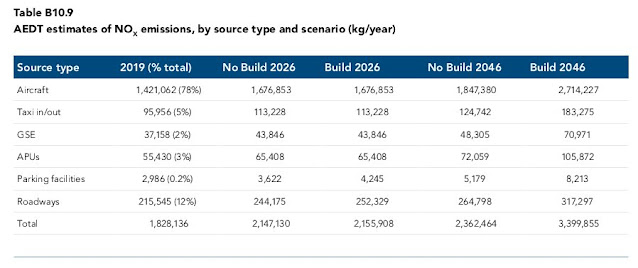 |
| Melbourne Airport MDP: NOx emissions |
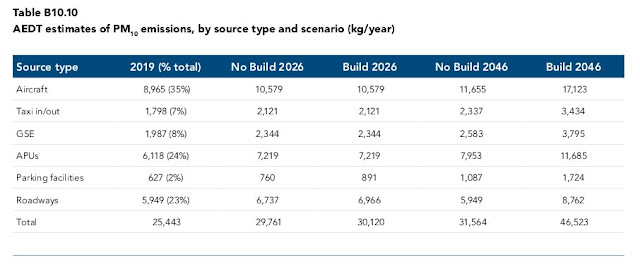 |
| Melbourne Airport MDP: PM10 emissions |
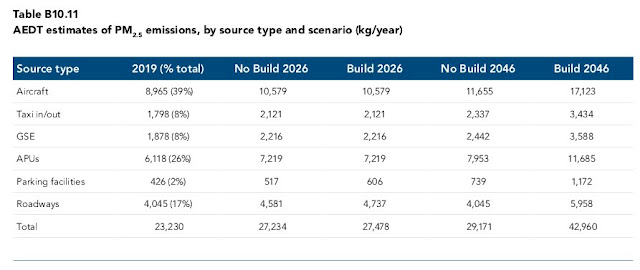 |
| Melbourne Airport MDP: PM2.5 emissions |
 |
| Melbourne Airport MDP: VOCs emissions |
Ultrafine particulates all fall into the PM2.5 emissions category. The strange thing about the PM10 and PM2.5 emissions readings for Aircraft and Taxi in/out is they have exactly the same readings. While all PM2.5 particulates can be classified as in the PM10 range, the reverse is not true. Are Melbourne airport trying to hoodwink us with these dodgy figures?
It gets even stranger when the MDP explains:
B10.7.6.3PM 2.5Predicted impacts of PM 2.5 emissions at the airport will closely follow predicted impacts for PM 10 since 100 per cent of PM 10 is PM 2.5 from airport sources. While PM 2.5 has a stricter criterion (25 µg/m 3 compared to 50 µg/m 3 for PM 10 ), model results demonstrate this criterion is met for all scenarios in all modelled years outside the airport boundary.
Most PM2.5 will not be PM10. It is a smaller particulate. Major Development Plan shows. No AEROMOD atmospheric dispersion modelling shown for PM2.5 pollution at all. Ultra Fine Particulates (UFP) are particularly important to model for health impacts and it appears Melbourne airport have not done this.
I would expect particulate pollution to be similar to Hudda et al (2014) and their findings for LAX, to follow downwind of the active flightpaths. Yes, meterological conditions may be slightly different, but the physics should be similar.
Noise Health Impacts
One of the health issues is the increase in noise pollution particularly under the flightpaths. This issue is already being taken up by local residents in the Northern suburbs. The Guardian reports that Melbourne residents opposed to Tullamarine airport’s $1.9bn proposed third runway say the federal government must implement an independent committee to review noise impacts.
Discussion
It is clear from a fairly shallow dive into the scientific literature that air pollution from aviation emissions has a large impact on air quality. This impacts human health from the local scale, around airports, to the global scale.
Building a third runway at Melbourne Tullamarine airport will induce more flights and increase aviation exhaust emissions which will affect air quality and human health.
Air quality will be affected over a much broader area than the noise contours, with likely up to 2 fold concentrations up to 16 kilometers downwind of flight paths, and five fold concentration up to 10km downwind according to the study for Los Angeles International. Yet the Major Development Plan for Melbourne does not show this particulate pollution dispersal.
References
- Bendtsen, K.M., Bengtsen, E., Saber, A.T. et al. A review of health effects associated with exposure to jet engine emissions in and around airports. Environ Health 20, 10 (2021). https://doi.org/10.1186/s12940-020-00690-y, https://ehjournal.biomedcentral.com/articles/10.1186/s12940-020-00690-y
- Dedoussi, Irene C. (2021), Implications of future atmospheric composition in decision-making for sustainable aviation, Environ. Res. Lett. 16 031002 https://iopscience.iop.org/article/10.1088/1748-9326/abe74d
- Harrison, R. M., Masiol, M., & Vardoulakis, S. (2015). Civil aviation, air pollution and human health. Environmental Research Letters, 10(4), 041001. https://iopscience.iop.org/article/10.1088/1748-9326/10/4/041001
- Hudda, Neelakshi, Tim Gould, Kris Hartin, Timothy V. Larson, and Scott A. Fruin,(2014), Emissions from an International Airport Increase Particle Number Concentrations 4-fold at 10 km Downwind, Environmental Science & Technology 2014 48 (12), 6628-6635 DOI: 10.1021/es5001566 https://pubs.acs.org/doi/abs/10.1021/es5001566
- Hudda, Neelakshi et al (2020), Impacts of Aviation Emissions on Near-Airport Residential Air Quality, Environ. Sci. Technol. 2020, 54, 14, 8580–8588, https://pubs.acs.org/doi/abs/10.1021/acs.est.0c01859
- Kwon, HS., Ryu, M.H. & Carlsten, C. Ultrafine particles: unique physicochemical properties relevant to health and disease. Exp Mol Med 52, 318–328 (2020). https://doi.org/10.1038/s12276-020-0405-1 https://www.nature.com/articles/s12276-020-0405-1
- Lammers et al (2020), Effects of short-term exposures to ultrafine particles near an airport in healthy subjects, Environment International, Volume 141, August 2020, 105779. https://www.sciencedirect.com/science/article/pii/S016041201934797X
- Wolfe, Philip J et al (2014), Near-airport distribution of the environmental costs of aviation, Transport Policy, Volume 34, July 2014, Pages 102-108. https://www.sciencedirect.com/science/article/pii/S0967070X14000547
- Yim, Steve H L et al (2015), Global, regional and local health impacts of civil aviation emissions, Environ. Res. Lett. 10 034001, https://iopscience.iop.org/article/10.1088/1748-9326/10/3/034001
Further Reading:
- Teddington Action Group, 7th December 2019, Emissions from Aircraft are harmful to us on the ground, http://www.teddingtonactiongroup.com/2019/12/07/are-emissions-from-aircraft-harmful-or-not/
- Union Européenne Contre les Nuisances Aériennes (UECNA) (European Union Against Aircraft Nuisances) - The Impact Of Ultra-Fine Particles https://www.uecna.eu/key-issues/emissions-health/impact-ultra-fine-particles-health/
- Lead image: An airplane takes off in California. Air travel emissions are a significant portion of all transportation emissions. Credit: dsleeter_2000/flickr




No comments:
Post a Comment